 Let me introduce myself. I’m Jenny from the UK; I’m originally from just outside Manchester but I now live in Hertfordshire near London. I suffered an AFE in April 2016 when I was 33 years old … this is my story. Let me introduce myself. I’m Jenny from the UK; I’m originally from just outside Manchester but I now live in Hertfordshire near London. I suffered an AFE in April 2016 when I was 33 years old … this is my story.
My partner and I tried for several months before I finally fell pregnant and we were so excited! This was my first pregnancy but my partner has a son from a previous relationship.
My pregnancy was going really well. We discovered at my 20 week scan that we were having a girl and we couldn’t have been happier! We were on Cloud 9.
I felt amazing, right up until week 32 when I developed obstetric cholestasis (OC). This made me feel quite unwell for a while until the medication I was prescribed began to help. I had to have weekly bloods and twice weekly monitoring of the baby meaning I took a month of sick leave before my maternity leave began. During this time, I had a few episodes of reduced movement and due to this combined with the OC the consultants decided to induce my labour at 38 weeks. By the time I was induced my bile levels were normal and my LFT also normal.
My partner and I went in at 8:00am a Monday and after waiting around all morning, I finally began the induction process. I had a 24 hour pessary followed by one lot of gel – after a while and with lots of walks round the hospital grounds, at around 2:00am on the Wednesday morning I was finally classed as in early labour and we moved to the labour ward.
Things were progressing very slowly and at around 4:50am, the midwife checked my cervix and as I was still only 4cm dilated, the decision was made to break my waters, which I found unbearably painful. This is when it all went wrong.
I now know that my uterus was hyper stimulating but at the time I didn’t have a clue what was happening and felt terrified; the pain went from completely manageable to horrifically unbearable in seconds. The next minute the emergency button was pressed, there were lots of doctors, consultants and midwives in the room and I was being told I needed to calm down as my baby was in distress – her heartbeat was dangerously low and wasn’t recovering. There’s nothing like hearing those words to bring you back into the room to focus!
I was rushed to theatre for an emergency c-section but once on the operating table and while preparations were being made, I screamed that I could feel pressure and on checking I was now 10cm dilated and my baby was crowning! I had gone from 4cm to 10cm in a matter of minutes which explained the horrific pain I was in!
The consultant rushed back into theatre and my daughter was born vaginally, on the operating table, at 5:42am after a ventouse assisted delivery. The de-briefing notes stated that she was ‘in poor condition’ from being starved of oxygen. We saw her for only a split second as she was quickly taken over to the other side of the room to get her breathing properly, it was the most awful thing to witness and I was completely helpless to do anything. Once they were happy with her breathing she was rushed to the neonatal ward and we were informed that they would be transferring her to another London hospital equipped for cooling treatment once they had stabilised her.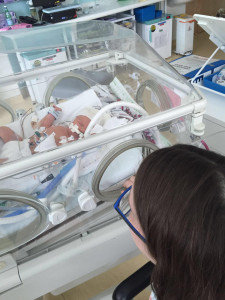
While all of this was happening with my daughter, the placenta had been delivered and I was stitched up and taken back to my room. Within minutes I began to feel that something wasn’t right, I didn’t feel very well and I felt that I was bleeding heavier than I should have been, I then vomited and this contained streaks of blood. My partner rushed out of the room and told the student midwife who then got the senior midwife and the consultants were called back quickly. It was discovered that my uterus wasn’t contracting and I was beginning to haemorrhage. I was taken straight back to theatre feeling very weak, frightened and disorientated; I had an epidural and the consultants tried to find out where the bleeding was coming from vaginally. Soon after this I began to feel very anxious and extremely agitated and my breathing became shallow. I remember saying to my partner who was in theatre with me “I feel sleepy but I’m scared if I go to sleep I won’t wake up!” This is the last thing I remember because the decision was made to put me under general anaesthetic so I could be operated on and I drifted off.
I awoke many hours later in intensive care, and the very first thing I remember thinking was “oh my god! I’m alive” and I remember being overwhelmed with relief but also very confused as to what was going on around me and at what had just happened.
Once I was stabilised, my partner was able to come in to see me. He brought in a couple of photographs of our daughter taken just before she had been transferred by ambulance to a different hospital which I kept with me … he also told me that all my family had travelled down to London from Manchester to be at the hospital as they had all been told that I might not make it through the surgery. At the time I don’t think I grasped the seriousness of it all but I was grateful that they were here for me.
During my time in intensive care, nothing was explained and I was left feeling alone and confused. That is until the consultant who delivered my baby and began my surgery called in to see me on a personal visit. He couldn’t believe that nobody had informed me about what had happened, and this was the first time a possible AFE was mentioned.
Apparently, I had a laparotomy and the surgeons had tried everything to stop the bleeding but nothing was working, they did b-lynch sutures and a bakri balloon but it continued, the final step was artery embolization which thankfully worked. This meant I was spared having to have a hysterectomy for which I will be eternally grateful. I had lost 5.5 litres of blood during my ordeal and required lots of blood, plasma and platelet transfusions. He told me I was very lucky to be alive and that they suspected it was an Amniotic Fluid Embolism. The words meant nothing to me, I was just so grateful to all the medical staff who had quite obviously saved my life.
I spent a few agonising days on the ward. My partner visited our daughter at the other hospital every day and would come to see me afterwards to give me updates. She was having cooling treatment for the lack of oxygen she suffered during the birth and was completely sedated but doing well. I cried uncontrollably every day, my heart ached at not being able to see or hold my baby but I was too poorly to be moved. Eventually I managed to convince the consultants to allow me to be transferred to where my daughter was. She was 4 days old when I first saw her, tiny and vulnerable in her incubator, hooked up to all sorts of beeping machinery. I was so weak and anaemic from the surgery and transfusions that I had to be wheeled down to see her and could manage no more than half an hour but it was worth every second!
Once our daughter had been taken out of ICU, she had an MRI scan and the results confirmed that there had been no brain damage at birth, she was completely fine – you can only imagine the tears of joy! My daughter and I recovered remarkably quickly and were home after just 10 days. This is when we began to attempt to come to terms with everything that had happened and to finally enjoy being mummy and daddy.
 AFE wasn’t mentioned to me again and I didn’t really take on board the possibility of having suffered with one but when I got home I did read a little bit about it and I didn’t believe that this had happened to me. It happened after the birth? I had no cardiac arrest? I hadn’t collapsed? I haemorrhaged before anything else happened? It didn’t add up. So I dismissed it completely. I was convinced that my waters shouldn’t have been broken and I blamed the hospital for this causing the massive haemorrhage. AFE wasn’t mentioned to me again and I didn’t really take on board the possibility of having suffered with one but when I got home I did read a little bit about it and I didn’t believe that this had happened to me. It happened after the birth? I had no cardiac arrest? I hadn’t collapsed? I haemorrhaged before anything else happened? It didn’t add up. So I dismissed it completely. I was convinced that my waters shouldn’t have been broken and I blamed the hospital for this causing the massive haemorrhage.
Four months on and I hadn’t received any contact regarding the report and de-briefing I had been promised by the hospital nor had I had any form of follow up appointment. When I chased this up through my GP I received a phone call from the Quality Governance Manager of the hospital. She informed me that it had been confirmed as an AFE and her words were “I shiver every time I read your notes”. It is this phone call that made me realise that it was very serious and I began to research AFE in more depth which dragged me into a further state of utter confusion and emotional turmoil.
I was having daily flash backs, horrific thoughts and was in a vicious cycle of dark emotions because I had so many unanswered questions. I got an infection at the surgery site, was weak with anaemia and felt completely disconnected from my baby, I was really struggling to bond. It wasn’t until she was around 9/10 weeks old that I started to feel like she was mine. I’m not sure I’ll ever get over the upset of those first few weeks and the immense guilt I feel about not having been there emotionally for her when she first came home.
The report and de-briefing helped me immensely. Everything was explained to me in detail. It turns out that I developed DIC and hypotension; because of this along with other unexplained factors, it became obvious that it was more than a haemorrhage alone and so by the process of elimination it has been confirmed that it was an AFE.
I feel relieved at being able to say I know what happened and I no longer feel anyone was to blame. It was an unpredictable and very unfortunate case of bad luck! I would certainly love for more research to be done into whether OC and / or induction of labour are linked to cases of AFE and if any of any those things could have been a contributing factor. None of these questions could be answered during my de-briefing.
The flashbacks and awful thoughts and feelings have subsided, however I think if we are to decide we would like another baby in the future this may be when I need to reach out and get some professional help. I’m not sure either my partner or I would cope well during another pregnancy but until that time comes, if it ever does, we refuse to worry.
It’s been a rollercoaster of a year! I am so grateful I finally found the courage to join the AFE Foundation support group. I had looked at it numerous times but couldn’t bring myself to join, I’m so pleased I have now. It’s been a huge help and support so far.
It’s now coming up to my daughter’s first birthday but I cannot allow myself to think “what if’s”. I am just so thankful to the amazing NHS medical team who were on call that day and who saved the lives of both me and my beautiful daughter. Our daughter’s first birthday will mean so much more than we could ever have imagined. |